HEALTH
Kidney Transplant Overseas: Better Blood & Creatinine Level
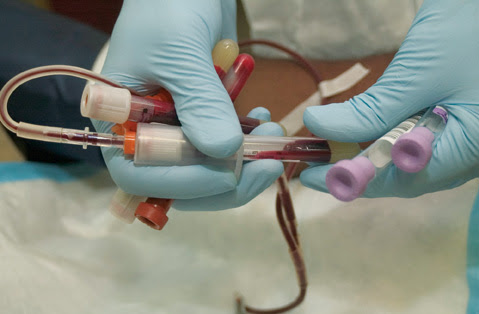
Kidney Transplant Benefits
Kidney transplantation is a life-saving procedure that offers hope to patients with end-stage renal disease (ESRD). With advancements in nephrology, kidney transplants have become an effective method to purify blood and control creatinine levels. In this article, I will discuss the benefits of kidney transplantation, its impact on blood purity, its effect on creatinine levels, and how it compares to dialysis.
Impact on Blood Purity
The kidneys play a crucial role in filtering waste and excess substances from the blood, maintaining blood salt and material balance, and regulating blood pressure, hormones, and levels of calcium and phosphorus essential for bone health. Kidney failure leads to a build-up of toxins and waste in the blood, resulting in high creatinine levels. A kidney transplant surgery from a kidney transplant center can effectively purify the blood by efficiently filtering toxins, waste, and excess fluids. With improved blood purification, patients experience a significant improvement in their overall well-being.
Effect on Creatinine Levels
Creatinine is a waste product generated by muscle metabolism. Elevated levels of creatinine in the blood indicate poor kidney function. Kidney transplantation leads to a significant reduction in blood creatinine levels. By replacing the failed kidney with a healthy donor kidney, the transplanted kidney efficiently filters creatinine from the blood. This reduction in creatinine levels not only helps in maintaining kidney function but also prevents the adverse consequences associated with high creatinine levels.
Comparison with Dialysis
While dialysis is a life-saving treatment for ESRD patients, it has limitations and can be time-consuming. Dialysis serves as a partial substitute for renal filtration and requires patients to undergo treatment regularly to remove waste and excess fluid from their bodies.
In contrast, a kidney transplant is a game-changer, providing a long-lasting solution to kidney failure. By receiving a healthy donor kidney, patients can live more normally and actively, eliminating the need for dialysis. Kidney transplantation, particularly overseas, offers improved blood purification, lower creatinine levels, and an overall better quality of life.
Medical Advancements in Kidney Transplantation
Over the years, medical advancements in kidney transplant overseas have greatly improved patient outcomes. Let’s explore some of these advancements, including enhanced blood filtration, improved metabolic balance, and a reduced risk of cardiovascular diseases.
Enhanced Blood Filtration
One of the significant benefits of kidney transplantation is the improved filtration capacity of the transplanted kidney. The new kidney efficiently filters toxins, waste, and excess fluids from the blood, leading to a rapid improvement in kidney failure symptoms. This enhanced blood filtration plays a crucial role in maintaining overall health and well-being.
Cardiovascular Risk Reduction
Chronic kidney disease patients are prone to various cardiovascular illnesses.
However, effective blood purification through kidney transplantation significantly minimizes the risk of such diseases. By reducing toxins and waste in the blood, a kidney transplant can alleviate strain on the heart and blood vessels, thereby improving cardiovascular health. This reduction in cardiovascular risk is a crucial benefit of kidney transplantation.
Creatinine Management in Transplant Patients
Managing creatinine levels is vital for the success of a kidney transplant. Let’s explore how kidney transplantation facilitates efficient waste management, allows for monitoring of kidney function, and emphasizes personalized medical approaches.
Waste Management Efficiency
A successful kidney transplant leads to a significant reduction in blood creatinine levels. By replacing the failed kidney, the transplanted kidney effectively manages waste in the body. High creatinine levels indicate poor kidney function, and controlling them is essential for the long-term health of transplant recipients. With a healthy transplanted kidney, waste management becomes more efficient, resulting in lower creatinine levels.
Monitoring Kidney Function
After a kidney transplant, regular monitoring of creatinine levels is crucial to assess the health and function of the transplanted kidney. Stable and low creatinine values indicate a healthy transplant, allowing for prompt treatment in case of any issues. By closely tracking creatinine levels, healthcare professionals can provide appropriate interventions to ensure the long-term success of the kidney transplant.
Personalized Medical Approach
To optimize the function and longevity of a transplanted kidney, personalized medical management is crucial. Immunosuppressive drugs are commonly prescribed to reduce the risk of kidney transplant rejection. These drugs not only help in preventing rejection but also optimize the function of the transplanted kidney and control creatinine levels. Long-term success after a kidney transplant heavily relies on tailoring the medical approach according to the individual’s needs.
Innovations in Kidney Transplant Procedures
Advancements in surgical techniques, improvements in donor matching, and a focus on post-transplant care have revolutionized kidney transplant procedures. Let’s explore these innovations in detail.
Surgical Enhancements
Kidney transplant success rates have significantly improved due to surgical breakthroughs. Minimally invasive procedures have reduced recovery time and complications, leading to better patient outcomes. These advancements in surgical techniques have made kidney transplantation a safer and more reliable option for ESRD patients.
Donor Matching Improvements
Genetic and immunological testing have played a vital role in improving donor matching for kidney transplantation. Better matching between donors and recipients reduces the risk of organ rejection and increases the survival rate of transplanted kidneys. By improving overall renal function, better donor matching also enhances creatinine management in transplant patients.
Focus on Post-Transplant Care
Regular monitoring and tailored drug regimes and diet have significantly improved post kidney transplant care. Close monitoring allows healthcare professionals to detect any potential complications or issues with the transplanted kidney at an early stage. This proactive approach enables quick interventions to maintain optimal renal function and improve long-term transplant outcomes.
Conclusion
Kidney transplantation offers numerous benefits to patients with end-stage renal disease. By purifying the blood and controlling creatinine levels, this life-changing procedure significantly improves the quality of life for individuals suffering from kidney failure. With advancements in surgical techniques, improved donor matching, and a focus on post-transplant care, kidney transplantation has become a more accessible and successful treatment option. Ongoing research and technological advancements provide hope for even better outcomes in the future. Thanks to these advancements, kidney transplant recipients can look forward to longer, healthier lives.
HEALTH
12 Common Triggers for Addiction and How to Avoid Them

Understanding and avoiding common triggers is essential for maintaining sobriety during addiction recovery. Triggers can lead to cravings and relapse if not managed effectively.
1. Stress
Stress is one of the most common triggers for addiction. High levels of stress can lead to cravings as individuals seek relief through substance use.
How to Avoid It:
Practice stress management techniques such as mindfulness, deep breathing exercises, and regular physical activity. Prioritize self-care and seek support from friends, family, or a therapist to help manage stress effectively.
2. Social Pressure
Social situations where others are using substances can be challenging for someone in recovery. Peer pressure can tempt you to join in and relapse.
How to Avoid It:
Surround yourself with supportive, sober friends. Politely decline invitations to events where substance use will be present. Plan alternative activities with friends who respect your commitment to sobriety.
3. Emotional Distress
Feelings of sadness, anger, or loneliness can trigger cravings for substances as a way to cope with negative emotions.
How to Avoid It:
Develop healthy coping mechanisms such as journaling, talking to a therapist, or engaging in a hobby. Build a strong support network to lean on during times of emotional distress.
4. Environmental Cues
Certain places, people, or situations associated with past substance use can trigger cravings.
How to Avoid It:
Identify and avoid high-risk environments that remind you of your substance use. Create new, positive associations by spending time in supportive, sober settings.
5. Celebrations and Holidays
Special occasions often involve substance use, which can be a trigger for those in recovery.
How to Avoid It:
Plan ahead for celebrations and holidays by bringing your own non-alcoholic beverages and having an exit strategy if you feel uncomfortable. Attend sober events or host your own celebrations without substances.
6. Fatigue
Being overly tired can lower your defenses and make it harder to resist cravings.
How to Avoid It:
Prioritize getting enough sleep and establish a regular sleep routine. Listen to your body and rest when needed to maintain physical and mental health.
7. Boredom
Idle time and lack of stimulation can lead to thoughts of substance use as a way to pass the time.
How to Avoid It:
Stay busy with activities that interest you, such as hobbies, exercise, or volunteering. Create a daily schedule to keep yourself engaged and productive.
8. Relationship Problems
Conflict and tension in relationships can trigger emotional distress and cravings.
How to Avoid It:
Practice open communication and seek therapy to address relationship issues. Surround yourself with supportive people who respect your recovery journey.
9. Physical Pain
Chronic pain or discomfort can lead to the temptation to use substances for relief.
How to Avoid It:
Work with healthcare professionals to manage pain through non-addictive medications and alternative therapies such as physical therapy, acupuncture, or mindfulness.
10. Financial Stress
Worrying about money can create significant stress, leading to cravings.
How to Avoid It:
Create a budget and seek financial advice to manage your finances effectively. Focus on building financial stability and seek support from friends, family, or financial counselors.
11. Celebrating Milestones
Ironically, achieving significant milestones in recovery can sometimes trigger thoughts of “rewarding” yourself with substances.
How to Avoid It:
Celebrate milestones in healthy, substance-free ways. Treat yourself to a special outing, a new hobby, or a meaningful experience that reinforces your commitment to sobriety.
12. Complacency
Becoming too comfortable in your recovery can lead to overconfidence and a lapse in vigilance, increasing the risk of relapse.
How to Avoid It:
Stay committed to your recovery routine and continue attending support groups and therapy sessions. Regularly review your goals and progress to stay focused on your sobriety.
Strategies for Managing Triggers
While avoiding triggers entirely may not always be possible, having strategies in place can help you manage them effectively. Here are some additional tips for managing triggers:
1. Develop a Relapse Prevention Plan
Create a detailed plan that outlines how you will handle triggers and cravings. Include specific strategies, coping mechanisms, and emergency contacts. Having a plan in place provides a sense of security and readiness.
2. Practice Mindfulness
Mindfulness involves staying present and aware of your thoughts and feelings without judgment. Practicing mindfulness can help you recognize triggers early and respond to them in a healthy way.
3. Build a Support Network
Surround yourself with supportive friends, family, and peers who understand your journey and can provide encouragement and accountability. Regularly attend support group meetings to stay connected and motivated.
4. Engage in Healthy Activities
Regular exercise, hobbies, and other positive activities can provide a healthy distraction from cravings. Engaging in activities that you enjoy helps build a fulfilling, sober lifestyle.
5. Seek Professional Help
Therapists and counselors can provide valuable support and guidance in managing triggers. Cognitive-behavioral therapy (CBT) and other therapeutic approaches can help you develop effective coping strategies.
6. Reflect and Adjust
Regularly reflect on your progress and the effectiveness of your strategies. Adjust your plan as needed based on your experiences and challenges. Continuous self-awareness and adaptability are key to maintaining sobriety.
7. Stay Educated
Educate yourself about addiction and recovery. Understanding the science behind addiction and learning about different recovery strategies can empower you to make informed decisions about your health.
8. Practice Self-Care
Prioritize self-care to maintain your physical and mental health. Taking care of yourself ensures you have the energy and resilience to handle triggers effectively.
9. Celebrate Progress
Acknowledge and celebrate your achievements, no matter how small. Recognizing your progress reinforces positive behavior and motivates you to continue your recovery journey.
HEALTH
Navigating the Costs of Live-In Dementia Care: A Guide for Families in the UK

Families seeking live-in dementia care costs in the UK face a complex and often daunting journey. With the prevalence of dementia rising and the demand for specialized care increasing, understanding the financial aspects of this endeavor is crucial. In this comprehensive guide, we’ll delve into the various factors influencing the costs of live-in dementia care in the UK and provide insights to help families make informed decisions.
Understanding the Need for Live-In Dementia Care:
Dementia is a progressive condition that affects millions of people worldwide, and the UK is no exception. As the condition advances, individuals often require round-the-clock supervision and support to ensure their safety and well-being. This level of care is typically provided through live-in arrangements, where trained professionals reside with the individual in need.
Factors Influencing Live-In Dementia Care Costs:
- Level of Care Required:
The cost of live-in dementia care in the UK varies depending on the individual’s specific needs. Factors such as the stage of dementia, level of cognitive impairment, and any additional medical or behavioral complexities can impact the required level of care and, consequently, the associated costs.
- Location:
Geographical location plays a significant role in determining the cost of live-in dementia care. Urban areas tend to have higher living expenses and thus may incur higher care costs compared to rural areas. Additionally, regional variations in care provider rates and availability can also influence pricing.
- Care Provider:
When seeking live-in dementia care, families have the option of choosing between private care agencies, independent caregivers, or residential care facilities. Each option has its own set of costs, with private agencies typically charging higher rates but offering comprehensive support and supervision.
- Additional Services:
Beyond basic caregiving, families may opt for additional services such as medication management, specialized therapies, or companionship programs. These supplementary services can enhance the quality of life for individuals with dementia but may incur extra expenses.
- Exploring Cost Estimates:
The cost of live-in dementia care in the UK can vary widely depending on the aforementioned factors. On average, families can expect to pay anywhere from £700 to £1500 per week for full-time, live-in care. However, this estimate is just a starting point, and actual costs may be higher or lower based on individual circumstances.
- Facility Amenities:
For residential care, amenities such as private rooms, recreational activities, and therapeutic programs can influence costs.
- Specialized Programs:
Facilities or caregivers offering specialized dementia programs, such as music therapy or sensory stimulation, may charge higher rates.
- Contract Terms:
Long-term contracts or flexible arrangements (e.g., hourly vs. daily rates) can impact cost structures.
- Caregiver Turnover:
High turnover rates among caregivers can affect the consistency of care and potentially increase costs due to retraining or recruitment efforts.
- Insurance Coverage:
The extent to which dementia care services are covered by health insurance or long-term care insurance policies can affect out-of-pocket expenses.
- Regulatory Requirements:
Compliance with local regulations and licensing standards can influence care providers’ operating costs, which may be reflected in pricing.
- Economic Factors:
Overall economic conditions, inflation rates, and labor market dynamics in a particular region can affect caregiver wages and service costs.
- Duration of Care:
Whether care is needed on a part-time, full-time, or 24/7 basis significantly impacts overall costs.
- Caregiver-to-Client Ratio:
Lower caregiver-to-client ratios, often found in premium services, can increase costs due to more personalized attention.
Navigating Financial Assistance Options:
- Local Authority Funding:
In some cases, individuals with dementia may be eligible for financial assistance from their local authority to cover care costs. However, eligibility criteria vary depending on factors such as income, assets, and level of need.
- NHS Continuing Healthcare:
NHS Continuing Healthcare is a funding package provided by the National Health Service (NHS) for individuals with complex medical needs, including those with advanced dementia. Eligibility assessments determine whether individuals qualify for fully funded care.
- Means-Tested Benefits:
Families may also explore means-tested benefits such as Attendance Allowance or Personal Independence Payment to help offset the costs of live-in dementia care. These benefits are designed to provide financial support to individuals who require assistance with daily living activities due to a long-term health condition.
Navigating the costs of live-in dementia care in the UK can be challenging, but with careful planning and research, families can make informed decisions that prioritize the well-being of their loved ones. By considering factors such as the level of care required, location, care provider options, and available financial assistance, families can create a sustainable care plan that meets their needs and budget. Ultimately, the goal is to ensure that individuals with dementia receive the support and dignity they deserve as they navigate this challenging journey.
HEALTH
Ways to Combat Loneliness in Addiction Recovery

Overcoming loneliness is a critical aspect of the addiction recovery process. The journey toward sobriety can lead individuals through uncharted and often daunting paths, where the lack of a supportive community may intensify feelings of isolation. However, overcoming loneliness, though challenging, is not impossible. By implementing targeted strategies and actively seeking out communities that offer support, individuals can discover both comfort and empowerment through increased connectivity. This article explores various approaches aimed at addressing loneliness, providing practical tips and insights to enhance interpersonal connections and promote emotional healing.
The road to recovery is seldom walked alone, and the feelings of detachment that often accompany it can be alleviated by connecting with others who understand the struggle. Establishing a network of support not only helps mitigate the sense of isolation but also reinforces the individual’s journey to sobriety with encouragement and solidarity. Engaging with groups and individuals who share similar experiences can provide a sense of belonging, making the path less intimidating. By exploring various tactics to overcome loneliness, this discussion offers valuable guidance to help individuals forge meaningful relationships and rediscover purpose in their recovery journey.
1. Embracing Support Groups:
Joining support groups is one of the most effective ways to combat loneliness during the recovery from alcohol and drug addiction. Well-known groups like Alcoholics Anonymous (AA) and Narcotics Anonymous (NA) offer a welcoming and empathetic setting where people can openly discuss their difficulties, achievements, and experiences. This openness is possible because these settings are designed to be judgment-free zones, ensuring that everyone feels secure and validated in sharing their personal stories. Active participation in these groups provides essential emotional support and helps individuals forge strong bonds of friendship and mutual understanding. The sense of community and connection that develops is invaluable, helping members to feel less isolated and more supported in their individual paths to recovery.
Regular attendance at group meetings is crucial for maintaining these connections and reinforcing the understanding that no one is alone in their struggles against addiction. As members meet consistently, they build trust and familiarity with one another, which strengthens their resolve and supports their recovery journey. This continuous engagement helps to solidify the group’s role as a cornerstone of support for its members, offering both stability and encouragement. Over time, this community becomes a key resource for individuals seeking solace and understanding as they navigate the complexities of addiction recovery, continually reminding them that they are part of a supportive and caring network.
2. Cultivating Meaningful Relationships:
Developing and maintaining strong, meaningful connections is critical in fighting loneliness during the process of addiction recovery. The inclination to withdraw can be powerful, but actively seeking deeper connections with others can greatly improve one’s emotional health. This often includes reconnecting with family, longtime friends, or mentors who can offer the necessary support and empathy. Furthermore, forming new friendships with people who have similar interests and values can help foster a supportive community, enhancing feelings of inclusion and connectedness.
In expanding these relationships, it’s important to participate in activities that both parties enjoy or to join clubs and groups that align with one’s personal interests. Whether it’s a book club, a fitness class, or a local support group, being part of a community can reduce feelings of isolation. Taking part in regular meetups not only builds stronger relationships but also establishes a routine that can help anchor someone’s social life, making the recovery process less daunting and more supported. These connections provide a safety net of peers who understand the challenges of recovery and offer a nurturing environment for personal growth and healing.
3. Engaging in Healthy Activities:
Loneliness can find fertile ground in inactivity, emphasizing the importance for those in addiction recovery to remain busy with beneficial pursuits. Immersing oneself in hobbies, physical fitness, or community service serves dual purposes—it not only diverts attention from feelings of solitude but also builds a sense of accomplishment and satisfaction. Involvement in pursuits that enhance both physical health and mental state plays a critical role in increasing self-esteem and confidence. This empowerment helps individuals fend off loneliness and maintain their dedication to the goals of their recovery journey.
4. Seeking Professional Support:
Beyond the camaraderie of support groups, obtaining professional help is critical in overcoming loneliness during addiction recovery. Engaging with therapists, counselors, and support staff offers targeted assistance that is customized for each person’s particular situation. In therapy sessions, individuals have the opportunity to delve into the root causes of their loneliness and craft personalized strategies to manage these feelings. Access to a reliable professional during tough periods offers not only comfort but also a new outlook, helping to diminish the sense of being alone and despondent. This professional support can be an anchor, providing stability and guidance as one navigates the complexities of recovery, ensuring that they do not have to face their challenges in isolation.
5. Utilizing Technology for Connection:
In our modern, tech-driven world, the internet serves as a powerful tool for building connections and finding support. Platforms such as online forums, social media groups, and chat rooms offer virtual spaces where people in addiction recovery can meet peers who are also navigating similar paths. These online communities help users share their experiences and challenges, providing a sense of solidarity and understanding.
Moreover, advances in digital communication have made teletherapy and online support groups increasingly accessible. These resources are particularly valuable for those who might find it difficult to attend physical meetings due to logistical issues, health concerns, or personal preferences. Virtual meetings can be attended from anywhere, removing physical barriers and making it easier for individuals to find and maintain supportive networks without leaving their homes.
By embracing these technological tools, people in recovery can effectively find companionship and support, thereby reducing feelings of isolation and helping to combat loneliness as they work towards sobriety. This digital approach not only supports individuals in maintaining their recovery efforts but also enriches their journey with a constant stream of accessible resources and communal support.
6. Practicing Self-Compassion:
In the journey of addiction recovery, embracing self-compassion emerges as a crucial tool in combating the pervasive feelings of loneliness. It’s about extending the same kindness, understanding, and acceptance to oneself that one might readily offer to others, especially during the toughest moments. Rather than allowing oneself to be drowned in self-criticism and the relentless chatter of negative self-talk, individuals can fortify their sense of self-worth and inner strength by nurturing self-compassion. This journey may entail acknowledging and validating the full spectrum of one’s emotions, consciously practicing mindfulness and acts of self-care, and embracing the inherent imperfections that define the human experience.
By adopting this compassionate stance towards oneself, individuals can gradually chip away at the walls of loneliness that often enclose them. It’s a process of fostering a profound connection not just with others, but with one’s own essence. Through this lens of compassion and empathy, individuals find themselves less burdened by the weight of loneliness, and instead, they uncover a newfound sense of belonging and connection that enriches their journey of recovery.
Conclusion:
The journey of addiction recovery often brings forth the daunting challenge of loneliness, yet it is a challenge that can be overcome. Through various avenues such as immersing oneself in support groups, nurturing authentic connections, participating in activities that promote wellness, seeking guidance from professionals, leveraging the power of technology to stay connected, and extending compassion towards oneself, individuals can effectively address feelings of isolation and pave the way for healing on their path to sobriety. It’s important to acknowledge that the road to recovery is not meant to be traveled alone; by bravely reaching out for assistance and forming bonds with others who understand and support, individuals can take significant strides towards a future filled with brightness and fulfillment. Together, united in our shared experiences and aspirations, we can conquer loneliness and flourish in our journey of recovery.
FAQs
- What are some common signs of loneliness in addiction recovery?
- Loneliness can manifest in various ways, including feelings of emptiness, isolation, and a lack of connection with others. It may also be accompanied by symptoms such as sadness, anxiety, and low self-esteem.
- How can support groups help combat loneliness in addiction recovery?
- Support groups provide a safe and understanding environment where individuals can share their experiences, receive encouragement, and connect with others who are facing similar challenges. By participating in support groups like Alcoholics Anonymous (AA) or Narcotics Anonymous (NA), individuals can find camaraderie and support on their journey to sobriety.
- What are some strategies for cultivating meaningful relationships in addiction recovery?
- Cultivating meaningful relationships involves reaching out to family members, old friends, or trusted mentors who can provide support and understanding. Additionally, forming new friendships with individuals who share similar interests and values can create a sense of belonging and support.

 HOME IMPROVEMENT1 year ago
HOME IMPROVEMENT1 year agoThe Do’s and Don’ts of Renting Rubbish Bins for Your Next Renovation

 BUSINESS1 year ago
BUSINESS1 year agoExploring the Benefits of Commercial Printing

 HOME IMPROVEMENT11 months ago
HOME IMPROVEMENT11 months agoGet Your Grout to Gleam With These Easy-To-Follow Tips

 HEALTH11 months ago
HEALTH11 months agoThe Surprising Benefits of Weight Loss Peptides You Need to Know

 TECHNOLOGY1 year ago
TECHNOLOGY1 year agoDizipal 608: The Tech Revolution Redefined

 HEALTH10 months ago
HEALTH10 months agoYour Guide to Shedding Pounds in the Digital Age

 BUSINESS1 year ago
BUSINESS1 year agoBrand Visibility with Imprint Now and Custom Poly Mailers

 HEALTH1 year ago
HEALTH1 year agoHappy Hippo Kratom Reviews: Read Before You Buy!









