HEALTH
Tooth Replacement Options for Seniors: What You Need to Know
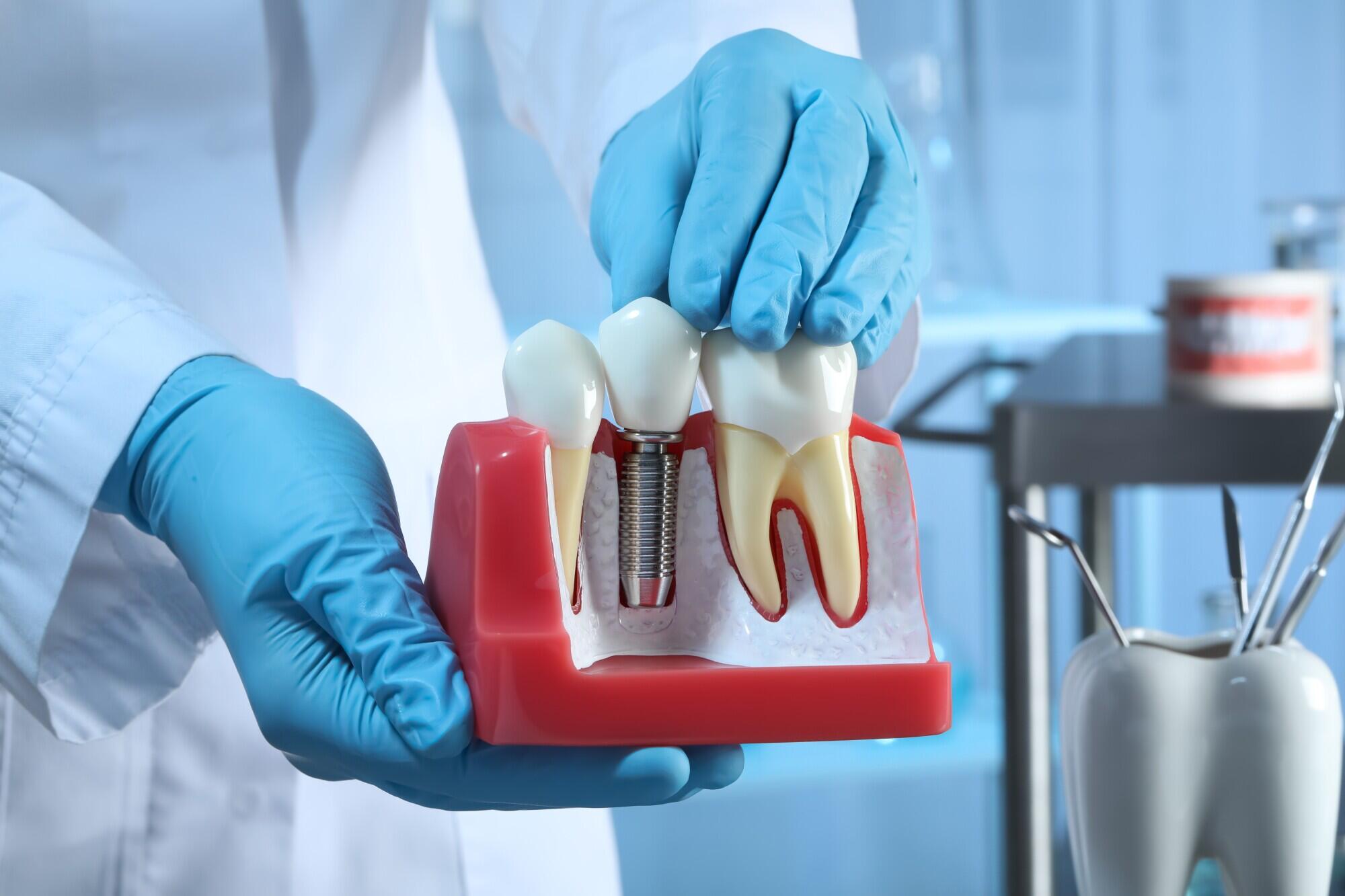
Did you know that the tooth replacement market is expected to reach $30.6 billion by 2031? This reflects the growing demand for tooth replacement options, particularly among seniors.
As we age, maintaining oral health becomes more important. Losing teeth can affect how we eat and our confidence.
For seniors, it is crucial to understand teeth replacement options. Each option has its benefits and considerations.
In this article, we will look at the tooth replacement options for seniors. Keep reading to learn more.
Dental Implants
Dental implants are often seen as the best choice for tooth replacement. Unlike dentures, implants are stable and permanent, improving oral function.
With a success rate of about 95%, implants can last a lifetime with proper care. This is helpful for seniors who want to enjoy their favorite foods without worrying about dentures slipping.
Implants also help prevent bone loss, which is important as we age. They feel and function like natural teeth. This makes them a great option for restoring confidence in your smile.
Implants can improve speech and comfort. They are easy to maintain with regular brushing and dental visits.
Who Is a Good Candidate?
Dental implants are a great option, but not everyone is a good candidate. Seniors with low bone density may need a procedure like bone grafting first. This helps ensure the implant will be successful.
It is important to talk to a dental professional to see if implants are right for you. They will consider your health and oral hygiene habits. Some may need additional treatments before getting implants.
Good oral care is key to the success of the implants. A dentist can help guide you through the process. They will make sure you are ready for the procedure.
The Procedure
The procedure for dental implants starts with a consultation with the dentist. The dentist will evaluate your oral health and decide if you are a good candidate.
The next step is placing the titanium post into the jawbone, which acts as a tooth root. After this, the post needs time to fuse with the bone, a process called osseointegration. This can take a few months.
Once the post is secure, the dentist will place a crown on top to complete the implant. The crown is custom-made to match your natural teeth.
Dentures
Dentures are a common choice for seniors. Modern dentures are more comfortable and look more natural than older ones. However, they need adjustments and replacements over time.
Despite this, dentures can improve quality of life by making it easier to eat and restoring facial appearance. They are also a cost-effective option for tooth replacement.
Dentures can be customized to fit your mouth perfectly. Regular dental checkups are important to keep them in good condition.
There are three types of dentures:
Complete Dentures
Complete dentures are used when all teeth are missing. They are custom-made to fit the gums perfectly.
Partial Dentures
Partial dentures are for people with some remaining natural teeth. They help create a more balanced bite and prevent the shifting of natural teeth. These dentures are designed to fit comfortably around the remaining teeth.
Implant-Supported Dentures
Implanted dentures combine the stability of implants with the convenience of dentures. They are fixed in place with dental implants, making them more secure than traditional dentures. This helps prevent slipping and improves chewing ability.
The Procedure
The procedure for dentures begins with a consultation with the dentist. The dentist will examine your mouth and discuss the best type of dentures for you. If necessary, any remaining teeth may be removed.
Impressions of your gums and remaining teeth are taken to create custom dentures. You will then be fitted with a temporary set while your permanent dentures are being made.
Once the dentures are ready, the dentist will check the fit and make adjustments. It may take some time to get used to wearing dentures. You will need to visit the dentist regularly for adjustments.
Bridges
Bridges are a middle ground between dentures and implants. They are more permanent than removable dentures but less invasive than implants. A bridge works by attaching an artificial tooth to nearby natural teeth or implants.
Bridges can improve appearance and function, but they may put pressure on the surrounding teeth. Over time, this can cause problems. Regular dental check-ups are needed to keep bridges in good shape.
Bridges can last for many years with proper care. They help restore the ability to chew and speak clearly. A dentist will monitor their condition to prevent issues.
The Procedure
Bridges are made from different materials, such as porcelain, metal, or a combination of both. The dentist will choose the best material based on your needs and preferences.
The procedure begins with preparing the adjacent teeth for support. Impressions are then taken to create a custom bridge. Once the bridge is ready, it is securely attached to the supporting teeth or implants.
The dentist will check the fit and make adjustments if necessary. After the procedure, it is important to maintain good oral hygiene. This is to ensure the bridge stays in good condition.
Comparing Options: What to Consider
When evaluating tooth replacement options, seniors should consider several factors:
Cost
Dental implants are more expensive at first, but they can save money over time. This is because they last longer than other options. Unlike dentures or bridges, implants do not need frequent replacement.
The durability of implants means fewer visits to the dentist for repairs or adjustments. While the initial cost is high, they provide a permanent solution to tooth loss. Other options like dentures may wear out or need replacements, which can add up.
Some dental insurance plans may cover part of the cost. Financing options are also available to help with the cost. It is important to weigh the long-term value when choosing the right option.
Maintenance
Dentures need regular adjustments and replacements, while implants are easier to maintain. Dentures may slip or feel uncomfortable over time. They need visits to the dentist for adjustments.
You also need to remove them for cleaning each day. Over time, dentures may wear down or lose their fit.
In contrast, implants do not need frequent visits for adjustments. This makes them more convenient. However, it is still important to visit the dentist for regular check-ups.
Comfort
Comfort varies from person to person. Some people prefer the fixed nature of implants over removable dentures.
Implants are natural-looking replacement teeth and do not move or slip. This makes them more comfortable for many people.
Dentures can feel bulky or uncomfortable, especially when eating or speaking. They may also cause irritation or sores in the mouth. It is important to discuss your comfort preferences with your dentist before making a decision.
Functional Limitations
Consider your food preferences, as some options may limit what you can eat. Dentures may make it harder to eat certain foods, like sticky or hard items. They may slip or feel uncomfortable while chewing.
With implants, you can eat a wider variety of foods because they are stable and strong. Bridges may also allow for more food choices, but they can put pressure on nearby teeth.
It is important to avoid certain foods with dentures, such as chewy candies or hard nuts. If you have dentures, you may need to cut food into smaller pieces.
Implants and bridges can help restore normal eating habits. Your dentist can guide you on how to maintain a healthy diet with your chosen tooth replacement.
Life After Tooth Replacement
Transitioning to any tooth replacement option can take time. For dental implants, recovery is important for successful healing.
Dentists provide instructions for aftercare, including food restrictions and oral hygiene. Following these guidelines helps ensure the implants integrate well with the bone.
For dentures, it may take time to get used to the feeling of something foreign in your mouth. Your dentist will advise on how long to wear them each day to help with the adjustment. Gradually wearing dentures helps the mouth adapt.
Regular cleaning is essential to prevent buildup and maintain hygiene. You will also need to visit the dentist for regular check-ups. These visits help ensure that the dentures are fitting well and not causing discomfort.
With proper care, both implants and dentures can last for many years. Regular maintenance helps keep the replacements in good condition. If any issues arise, your dentist can make adjustments to improve comfort.
Finding the Right Dental Professional
Choosing a qualified dentist who understands the needs of seniors is important. Whether you are considering implants, dentures, or bridges, a skilled dentist can guide you. Here are some tips to help you choose:
Look for a Dentist With Experience
Look for a dentist with experience working with seniors. They will understand the unique challenges seniors face with oral health. An experienced dentist can recommend the best tooth replacement options for your needs.
They are also more familiar with age-related conditions like bone loss or gum disease. This expertise can help ensure better outcomes for your treatment.
Always ask about their experience during your consultation. A dentist who specializes in senior care will make you feel more confident in your choice.
Check Reviews
Check reviews before choosing a dentist. Dental online reviews can give you insight into other experiences. Look for positive comments about the skill and care.
Pay attention to any repeated concerns or complaints. Reviews can also help you learn about the office staff and overall environment.
Ask friends or family for recommendations as well. Personal experiences can often provide valuable information. Taking time to read reviews can help you make a more informed choice.
Consider Their Communication Style
Consider the communication style when making your choice. A good dentist should take the time to listen to your concerns.
They should explain your options clearly and in simple terms. This helps you feel confident about your treatment plan.
If a dentist rushes through explanations or dismisses your questions, they may not be the right fit. Look for someone patient and approachable.
Clear communication is especially important for understanding procedures and aftercare. Feeling comfortable asking questions can improve your overall experience.
Make Sure the Office is Accessible
Make sure the dental office is easy to access. Check if it is located near your home or in a convenient area. Look for parking spaces or public transportation options nearby.
The office should also be senior-friendly, with ramps or elevators if needed. Inside, the waiting area should be comfortable and welcoming. Consider the office hours to ensure they fit your schedule.
Accessibility is important for regular visits and follow-up care. A convenient and comfortable office can make your dental experience much easier.
Consider the Cost and Payment Options
Consider the cost and payment options when choosing a dentist. Dental procedures can be expensive, so it is important to know what to expect. Ask if the dentist accepts your insurance plan or offers payment plans.
Some offices provide financing options to help manage costs. Check if there are any additional fees for consultations or follow-up visits. It is also a good idea to compare prices with other dental offices.
Understanding the costs upfront can help you plan your budget. Choosing a dentist with flexible payment options can make treatment more affordable.
Visit the Office
Visit the dental office before making your final decision. This allows you to see if the environment feels clean and welcoming. Pay attention to how the staff treats you during your visit.
Friendly and helpful staff can make a big difference in your experience. Check if the waiting area is comfortable and not overcrowded. Observe if the equipment and facilities look modern and well-maintained.
Visiting the office also gives you a chance to ask questions in person. It helps you decide if the office meets your needs and expectations. A positive first impression can give you confidence in your choice.
Tooth Replacement Options: Making an Informed Decision
Understanding the variety of tooth replacement options available empowers seniors to make informed decisions regarding their oral health. Each solution offers unique benefits designed to restore function and appearance.
Prioritize consultations with dental professionals who can provide tailored advice suited to individual needs. With the right support, seniors can find effective tooth replacement options that lead to a healthier, more confident smile. Now is the time to take the first step towards achieving your ideal dental health.
If you like to learn more, check out more articles on our blog.
HEALTH
Understanding in Which Compartment Would Fluid Accumulate in Edema

Do you notice that you have extra fluid in your extremities or other body parts when you wake up in the morning or at night?
Edema, characterized by the abnormal accumulation of fluid in the body’s tissues, is a common medical condition with various underlying causes and manifestations. To understand edema fully, it’s essential to grasp the mechanisms by which fluid accumulates and the compartments within the body where this accumulation occurs.
In this article, we’ll delve into the physiology of edema and explore the answer to the question, “In which compartment would fluid accumulate in edema?”
What Is Edema?
Edema refers to the excessive accumulation of fluid in interstitial spaces, leading to tissue swelling. It can occur locally, affecting specific body parts, or globally, involving multiple areas of the body.
Edema can be caused by various factors, including:
- Inflammation
- Impaired circulation
- Fluid retention
- Underlying medical conditions such as heart failure, kidney disease, or liver cirrhosis.
Is swelling of the legs sign of heart failure? If you are worried about it, then consult with your medical professional ASAP.
Here are the compartments of fluid distribution to consider.
Intravascular Compartment
The intravascular compartment, also known as the vascular space or bloodstream, consists of the blood vessels (arteries, veins, and capillaries) that circulate blood throughout the body.
In some cases, such as heart failure or liver disease, fluid may accumulate within the intravascular compartment due to increased hydrostatic pressure or decreased oncotic pressure. This leads to conditions like pulmonary edema or ascites.
Interstitial Compartment
The interstitial compartment refers to the space between cells and blood vessels. This is where interstitial fluid circulates and exchanges nutrients, waste products, and gases with surrounding tissues.
Edema primarily occurs within the interstitial compartment when fluid leaks out of blood vessels due to increased capillary hydrostatic pressure, decreased oncotic pressure, or impaired lymphatic drainage.
Common examples of interstitial edema include peripheral edema (swelling of the extremities) and dependent edema (fluid accumulation in dependent areas of the body due to gravity).
Intracellular Compartment
The intracellular compartment comprises the fluid contained within cells, which plays a crucial role in maintaining cellular function and homeostasis. While edema primarily affects the extracellular compartments (intravascular and interstitial), certain conditions, such as cellular injury or inflammation, may lead to intracellular edema, causing cells to swell and impairing their function.
Mechanisms of Fluid Accumulation in Edema
There are three reasons why fluid might accumulate in edema. It could be due to increased hydrostatic pressure within the blood vessels. This could be due to heart failure, venous insufficiency, or kidney disease.
Reduced oncotic pressure, attributed to hypoalbuminemia (low levels of albumin in the blood) or liver disease, diminishes the osmotic force that normally helps retain fluid within blood vessels, contributing to fluid leakage and interstitial edema.
Lymphatic drainage also might result in fluid accumulation.
In Which Compartment Would Fluid Accumulate in Edema?
It’s important to go to a medical professional as soon you notice fluid in your extremities or fluid accumulation due to edema. Don’t try to answer the question yourself, “In which compartment would fluid accumulate in edema?”
Browse through related articles on our website to stay informed on various subjects.
HEALTH
Hypokalemia ICD 10: A Guide to Symptoms and Medical Coding

Introduction to Hypokalemia icd 10
Hypokalemia ICD 10 might sound like a mouthful, but it’s an essential topic for anyone involved in healthcare or medical coding. Understanding this condition can make all the difference when diagnosing and treating patients effectively. Hypokalemia refers to low potassium levels in the blood, a situation that can lead to serious health issues if left unaddressed. As we dive into this guide, you’ll discover not only what hypokalemia is but also how it’s coded in the ICD-10 system. Whether you’re a healthcare provider or just curious about medical terminology, this overview will equip you with valuable insights into symptoms, diagnosis, and treatment options associated with hypokalemia. Let’s navigate through these vital details together!
What is Hypokalemia and How is it Diagnosed?
Hypokalemia is a condition characterized by low levels of potassium in the bloodstream. Potassium plays a vital role in numerous physiological processes, most notably in facilitating muscle movements and transmitting nerve impulses. When levels dip below normal, it can lead to significant health issues.
Diagnosis typically starts with a simple blood test. Healthcare professionals measure serum potassium levels to confirm hypokalemia. Normal potassium ranges from 3.5 to 5.0 mEq/L; anything lower indicates a problem.
Additionally, doctors may evaluate symptoms such as muscle weakness or fatigue that are common indicators of this condition. Sometimes, further tests are necessary if underlying causes—like kidney disorders or medication effects—are suspected.
Identifying the root cause is crucial for effective management and treatment strategies tailored to individual needs.
Symptoms of Hypokalemia
Hypokalemia manifests through a variety of symptoms that can significantly affect daily life. Patients may experience muscle weakness, which can range from mild fatigue to severe impairment in physical performance.
Cramps and spasms are also common complaints. These sudden contractions can be painful and often occur during exercise or at night.
Another notable symptom is irregular heart rhythm, known as arrhythmia. This condition poses risks for serious complications if left unaddressed.
Digestive issues like constipation may arise due to slowed bowel function. It’s essential to monitor these signs closely, as they could indicate worsening potassium levels.
Mental health isn’t immune either; anxiety and mood changes frequently accompany hypokalemia. Recognizing these diverse symptoms aids in timely diagnosis and treatment efforts.
Medical Coding for Hypokalemia
Medical coding for hypokalemia requires careful attention to detail. Accurate coding ensures proper documentation and reimbursement.
Hypokalemia is characterized by low potassium levels in the blood, which can lead to various health complications. Coders must understand the medical implications when assigning codes.
When documenting hypokalemia, it’s essential to capture not only the condition itself but also any underlying causes or related symptoms. This holistic approach enhances clarity and improves patient care tracking.
Specific guidelines exist within ICD-10 that address different manifestations of hypokalemia. Familiarity with these nuances helps coders select the most precise code.
Mistakes in coding can result in claim denials or delayed payments. Therefore, continuous education on updates in medical coding practices is vital for all professionals involved.
Commonly Used ICD-10 Codes for Hypokalemia
When it comes to coding hypokalemia, accuracy is crucial. The ICD-10 offers specific codes that healthcare professionals should familiarize themselves with.
The primary code for hypokalemia is E87.6, which covers unspecified causes of low potassium levels in the blood. This code is essential when the cause remains undiagnosed and needs further investigation.
For cases linked to chronic kidney disease, you might encounter additional codes like N18.x series, depending on the stage of the disease. If a patient has undergone diuretic therapy leading to hypokalemia, it’s important to note this as well using relevant medication-related codes.
Each situation can be unique; thus, precise documentation will support correct coding practices. Taking time to understand these nuances ensures appropriate patient care and accurate billing processes.
Tips for Accurate Medical Coding
Accurate medical coding is essential for proper diagnosis and billing. Start by ensuring you have the latest coding manuals at hand. Staying updated on any changes to ICD-10 codes can prevent costly errors.
Double-check all patient records before assigning a code. This includes reviewing lab results, physician notes, and any related diagnoses. Precision is paramount; even the smallest data point is critical for ensuring total accuracy in medical documentation.
Collaboration with healthcare providers plays a crucial role too. Clear communication helps clarify uncertainties about symptoms or treatments that directly impact coding.
Utilize software tools designed for medical coding assistance. These programs often highlight potential mistakes and suggest appropriate codes based on input data.
Regular audits of your coding practices can help identify patterns in errors. Learning from these insights strengthens overall proficiency in medical coding processes while enhancing compliance.
Treatment Options for Hypokalemia
Treatment for hypokalemia primarily focuses on restoring potassium levels in the body. This is crucial, as low potassium can lead to serious health issues.
Oral potassium supplements are often prescribed. These come in various forms, including tablets or powders. They allow for gradual replenishment of potassium levels over time.
In more severe cases, intravenous (IV) administration may be necessary. This method delivers potassium directly into the bloodstream for rapid results.
Nutritional intake is equally fundamental to the healing process, serving as a cornerstone for effective recovery. Foods rich in potassium like bananas, oranges, and spinach should be incorporated into daily meals.
Monitoring is key during treatment. Regular blood tests help ensure that potassium levels return to normal without exceeding safe limits.
Addressing underlying causes is equally important. Conditions such as kidney disease or certain medications might need adjustment for effective management of hypokalemia.
Conclusion
Hypokalemia, or low potassium levels in the blood, is a condition that requires attention due to its potential impact on health. Understanding its symptoms and accurate medical coding with ICD-10 can greatly aid healthcare providers in delivering effective treatment. Patients experiencing fatigue, muscle weakness, or irregular heartbeats should seek medical evaluation promptly.
Medical coding plays a critical role in documenting hypokalemia cases accurately. Using the correct ICD-10 codes ensures that healthcare facilities receive appropriate reimbursement while maintaining complete patient records. Familiarizing yourself with commonly used codes enhances workflow efficiency.
When treating hypokalemia, addressing the underlying cause is paramount. Whether through dietary changes or supplements, timely intervention can significantly improve outcomes for those affected.
A proactive approach towards understanding hypokalemia and mastering its coding will contribute positively to both patient care and administrative processes within healthcare systems.
HEALTH
The Ultimate Guide to Finding the Best Anti Aging Facial Treatment for Your Skin

Are you looking for the best way to keep your skin young and fresh?
With so many treatments available, it can be hard to know which one is right for you. In this guide, we will explore different anti aging facial treatments.
You will learn about their benefits and how they work. By the end, you will have all the information you need to make a smart choice.
Get ready to find the perfect treatment for your skin!
Understand Your Skin Type
Knowing your skin type is key to picking the right treatment. There are four main types: oily, dry, combination, and sensitive.
Oily skin gets shiny and may have large pores. Dry skin feels tight and might flake. Combination skin has both oily and dry spots. Sensitive skin can get red and irritated easily.
By knowing your type, you can choose a treatment that helps you get youthful skin. A good match will keep your skin looking fresh and glowing.
Research Ingredients
When choosing skincare products, it’s important to know what ingredients work best for your skin type. Look for products with retinol, which helps smooth fine lines, or hyaluronic acid, which keeps skin hydrated.
Vitamin C brightens and tones the skin. Avoid harsh chemicals that can cause irritation, especially if you have sensitive skin.
Read labels carefully and look for natural ingredients. This research will help you pick effective skincare products that support healthy, youthful skin.
Consult a Dermatologist
Before starting any anti aging treatment, it’s smart to talk to a dermatologist. They can check your skin and help you choose the best treatments. A dermatologist can recommend products and treatments that suit your specific skin type.
They also know about the latest techniques and can guide you in finding trusted botox experts if you’re interested in that option. By consulting a professional, you ensure that your skin gets the care and attention it needs to stay youthful and vibrant.
Read Reviews and Testimonials
Reading reviews and testimonials from others can help you find the best anti aging treatments. Look for feedback from people with similar skin types. They will give honest opinions about what worked for them and what didn’t.
Check multiple sources like skincare blogs, forums, and product websites. Pay attention to patterns in reviews, such as common praises or complaints. Doing this will save you time and money, and you’ll feel more confident choosing a treatment that others have found effective.
Start with a Patch Test
Before using any new skincare product, always do a patch test. Apply a small amount of the product on a tiny area of your skin, like behind your ear or on your wrist. Wait 24 hours to see if you get any reactions, such as redness or itching.
If your skin stays calm, you can use the product on your face. A patch test helps you avoid adverse reactions and ensures the product is safe for your skin type. This small step keeps your skin healthy and protected.
Find the Right Anti Aging Facial Treatment Today
Finding the right anti aging facial treatment requires some effort, but it’s worth it for youthful, glowing skin. Understand your skin type, check ingredients, consult a dermatologist, read reviews, and do a patch test.
These simple steps will guide you to a treatment that keeps your skin looking its best. Take action now for lasting beauty and confidence.
If you enjoyed this article please take the time to check out some of the other great content on our site.

 HOME IMPROVEMENT1 year ago
HOME IMPROVEMENT1 year agoThe Do’s and Don’ts of Renting Rubbish Bins for Your Next Renovation

 BUSINESS1 year ago
BUSINESS1 year agoExploring the Benefits of Commercial Printing

 HOME IMPROVEMENT9 months ago
HOME IMPROVEMENT9 months agoGet Your Grout to Gleam With These Easy-To-Follow Tips

 BUSINESS1 year ago
BUSINESS1 year agoBrand Visibility with Imprint Now and Custom Poly Mailers

 TECHNOLOGY12 months ago
TECHNOLOGY12 months agoDizipal 608: The Tech Revolution Redefined

 HEALTH9 months ago
HEALTH9 months agoThe Surprising Benefits of Weight Loss Peptides You Need to Know

 HEALTH9 months ago
HEALTH9 months agoYour Guide to Shedding Pounds in the Digital Age

 LAW1 year ago
LAW1 year ago7 Key Questions to Ask When Hiring a Criminal Lawyer









